ONJ is a very rare condition that can delay healing inside the mouth area. It can occur after a tooth extraction, dental disease, radiation therapy or for no apparent reason. It has occurred in some people taking some Osteoporosis medications and research shows that there may be a connection between ONJ and the following medications which are used to prevent bone loss: Risedronate, Ibandronate, Alendronate, Zoledronic acid and Denosumab.
Your risk of breaking multiple bones and losing your independence usually far outweighs your risk of developing ONJ and this would be why you have been prescribed to take any of the above listed medications.
Your risk of developing ONJ is very low, but you can reduce this risk by the following:
Your risk of developing ONJ is slightly higher:
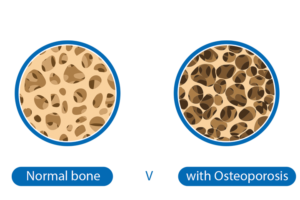
What is Osteoporosis?
Osteoporosis is a disease that affects the inside of your bones, making them fragile. The images above show how Osteoporosis causes large holes to develop in the inside of your bones, which is why they break easily. Broken bones are also known as fractures. Example: You have been told that you have fractured vertebrae/ collapsed vertebrae/crushed vertebrae, which all mean you have broken bones in your back.
What is Osteopenia?
Osteopenia is the early stages of Osteoporosis. Research shows that most broken bones (fractures) occur in the moderate to marked Osteopenia range, which is a DXA scan T score result of -1.5 to -2.49. FYI: A person can be diagnosed with Osteopenia in their hips and Osteoporosis in their back or the reverse.
Are Osteoporosis and Osteopenia treatable?
Yes, it is very rare when a person cannot improve their bones. We know of 90-year-olds who have improved their bone health.
The signs and symptoms of possible undiagnosed Osteoporosis
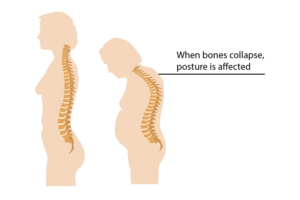
What can happen to a person if they have untreated Osteoporosis?
Untreated Osteoporosis can lead to a person breaking multiple bones, which can lead to disfigurement, pain, incontinence, and loss of independence. It is estimated that only 19% of people with bone loss are diagnosed, which is why it is so important that you check to see if you have risk factors for bone loss.
How is Osteoporosis diagnosed?
A DXA scan will show if you have lost bone, and a DXA scan of your spine and hips is the only test we recommend for screening and diagnosing Osteoporosis. A DXA scan takes 15 minutes, is painless and it is not claustrophobic. We recommend repeat DXA scanning to monitor your response to your Osteoporosis treatment, minimum every two years.

My DXA scan results have declined, what can I do?
Your DXA scan resutls should not decline, this must be investagated. There are many reasons why this can occur.
Which is the best Treatment for Osteoporosis?
There are different types of treatments for Osteoporosis and the best treatment for you will depend on your age, your DXA scan results, if you have broken bones or are high risk to break bones, your medical history and the most important, the causes of your bone loss.
Do you ever recommend treating Osteoporosis without a medication?
We are the National experts in Osteoporosis, and we only recommend treatments that have had extensive clinical research done on them to ensure they reduce your risk of breaking bones.
Calcium and Vitamin D
Calcum and Vitamin D are essential for helping to pevent bone loss, and also to improve your bone health, as well as overall health. We recommend that you try to get both from food, and only take a supplement if this is not possible.
Should a person with bone loss exercise?
Yes, but you need to be very careful what exercises and stretches you do. To stay independent, it is essential that you exercise but you should be assessed to see what exercises are safe and appropriate for you. Adults need 30 minutes of weight bearing exercise a day and children need 60 minutes of weight bearing exercise a day.
What exercises are NOT recommended for those with bone loss?
Many stretches in yoga, such as touching your toes with your legs straight. High impact step aerobics, trampolines and regular sit ups. Lifting heavy weights or objects, twisting your back with your feet not moving as your twist, skiing and vibrating machines. Senior citizens should not lift young babies or children, even if they do not have bone loss, as it is extremely unsafe for the grandparent and the child.

I want to prevent myself getting bone loss, what should I do?
Contact us for more information, as we are the National experts in Osteoporosis.
I have been diagnosed with Osteoporosis, what should I do?
Contact us for more information, as we are the National experts in Osteoporosis.
What about men?
Men are at a significant disadvantage when it comes to Osteoporosis because it is commonly perceived to be an older women’s disease. All men need to check if they have risk factors for bone loss, as men are at risk of Osteoporosis.