Calcium and vitamin D3 help to build strong bones and are essential for everyone throughout life.
Calcium helps to keep our bones healthy, our muscles, nerves, cells and our heart working properly, and help blood clots to form when we cut ourselves. 99% of the calcium in our bodies is in our bones and teeth.
Vitamin D3 is very important to help protect our bones, helping your body to absorb calcium and supporting your muscles to help decrease falls, as well as helping your immune system.
Vitamin D3 can be found in a few foods:
Oily fish such as salmon, tuna, sardines, mackerel, halibut and herring, are all excellent sources of vitamin D3. Eating oily fish twice a week can help get your vitamin D3, depending on the portion size.
Eggs contain Vitamin D3 and a lot of milk products and margarines are fortified with vitamin D3.
Breakfast cereals, soya milk and rice milk may also be fortified with vitamin D3.
Low Vitamin D levels are very common in Ireland
The lack of sunshine and the fact that only a few foods naturally contain vitamin D3.
We usually have some sunny days in May, June, July and August, so 15 minutes a day in the sun, then put sun block on. If you burn easily, please do not try to get your Vitamin D from the sun.
In the winter it is extremely important to make sure you are getting enough Vitamin D3.
In Ireland 74% of adults and 88% of primary school children, have less than half of the recommended daily amount of vitamin D.
Calcium can be found in some foods
Dairy products are one of the best sources of calcium (milk, cheese and yoghurt), especially the fortified milks, as they have calcium and vitamin D3. Bread, nuts, oily fish, sesame seeds, dried fruit, and tofu also contain calcium, as well as some dark green vegetables. Some brands of orange juice and most breakfast cereals have added calcium , Vitamin D3 and first class proteins.
How much calcium and Vitamin D3
Women and men 50+ years with bone loss = 1200 mg of Calcium per day
Women and men 50+ with bone loss = 20-30μ / 800-1000 IU of Vitamin D3 per day
*Note: There are Calcium and vitamin D3 supplements, as well as vitamin d supplements, but should only be taken by those who cannot get their daily amounts from food.
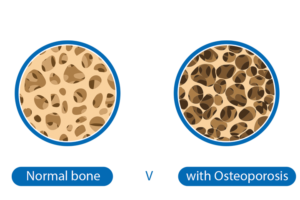
What is Osteoporosis?
Osteoporosis is a disease that affects the inside of your bones, making them fragile. The images above show how Osteoporosis causes large holes to develop in the inside of your bones, which is why they break easily. Broken bones are also known as fractures. Example: You have been told that you have fractured vertebrae/ collapsed vertebrae/crushed vertebrae, which all mean you have broken bones in your back.
What is Osteopenia?
Osteopenia is the early stages of Osteoporosis. Research shows that most broken bones (fractures) occur in the moderate to marked Osteopenia range, which is a DXA scan T score result of -1.5 to -2.49. FYI: A person can be diagnosed with Osteopenia in their hips and Osteoporosis in their back or the reverse.
Are Osteoporosis and Osteopenia treatable?
Yes, it is very rare when a person cannot improve their bones. We know of 90-year-olds who have improved their bone health.
Who is at risk of developing Osteoporosis?
Anyone can develop Osteoporosis, as it affects women and men of all age groups and can even affect children. You will not feel the insides of your bones getting thinner, which is why everyone should check to see if they have risk factors for bone loss. Women over 65 are the highest risk group affected as they will have gone through the menopause, which is when a significant amount of bone can be lost. 90% of fractured hips (broken hips) are due to Osteoporosis and 7 out of 10 hip fractures happen to women.
What are the risk factors for losing bone?
There are approximately 200 causes of bone loss. Some causes are secondary effects from other diseases, treatments for other diseases and others are lifestyle choices. The following are some of the many risk factors, the Menopause, Family history especially of a broken hip, Radiation, chemotherapy and some treatments for breast and prostate cancer. Rheumatoid arthritis, Coeliac disease/Gluten sensitivity and Low levels of sex hormones in females and males. Anorexia/Bulimia, over exercising, Lack of weight bearing exercise, many medications such as protein pump inhibitors, others that contain cortisone such as steroid asthmatic inhalers, some anti-depressants and some water pills, Low calcium and/or Vitamin d levels, Physiological or psychological stress, smoking and excess alcohol.
The signs and symptoms of possible undiagnosed Osteoporosis-